Bangladesh’s Measles Catastrophe: A Stark Warning for India’s Children
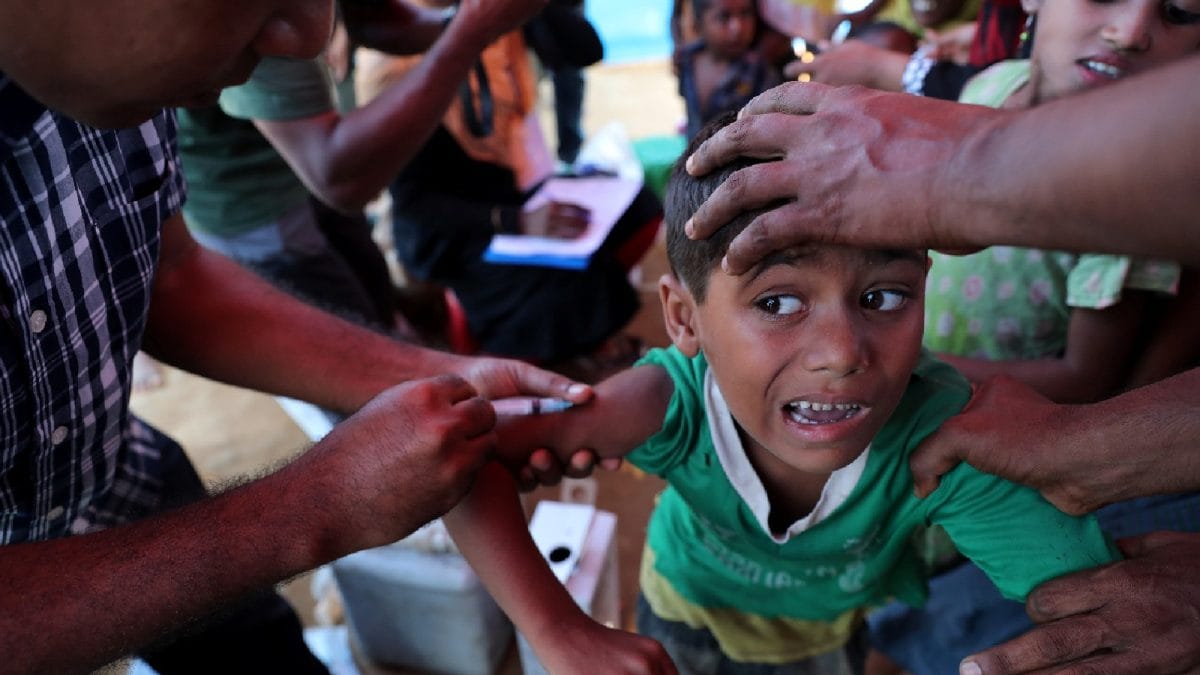
Bangladesh’s deadly measles surge shows how fast outbreaks return when vaccination dips — a warning for India, where immunity gaps could put children at risk.
At least ninety‑eight children have died in Bangladesh over a three‑week period as measles resurfaces with alarming speed. The disease, long perceived as a problem of the past, is now re‑emerging with deadly vigor, and children bear the brunt of the crisis.
Bangladesh’s Infectious Diseases Hospital in Dhaka, a facility originally designed to accommodate roughly one hundred patients, is rapidly approaching capacity limits. In the first months of the current year, doctors have reported two hundred fifty‑five pediatric admissions for measles, a sharp increase from the sixty‑nine cases recorded throughout the previous year. The surge has forced staff to place patients on the floor, convert corridors into makeshift wards, and stretch limited supplies to the breaking point.
The upward trajectory began in January and has only accelerated since, with a continuous flow of young patients arriving at the hospital’s doors. Each day, families travel from distant villages, seeking lifesaving treatment for children whose conditions deteriorate within hours of symptom onset.
Beyond the numbers, the human dimension of the outbreak is stark. Infants are being transferred from one facility to another, parents are left scrambling for any available bed, and overcrowded rooms have turned into emergency zones where medical personnel battle fatigue and resource scarcity.
Children Hit the Hardest by Measles
The current wave has proved especially lethal for children. The confirmed death toll of ninety‑eight youngsters paints a grim picture of measles’ potential to cause rapid, fatal outcomes when it spreads unchecked.
Medical data clarifies why children are disproportionately affected. In Bangladesh, five to six per cent of measles‑infected children develop pneumonia, a leading cause of measles‑related mortality. Additional research indicates that mortality rates can double among unvaccinated children, with some analyses reporting double‑digit fatality percentages within highly vulnerable groups.
Measles’ danger is not limited to the viral infection itself; complications such as pneumonia, severe dehydration, and immune system suppression amplify risk, particularly among children who are malnourished or who have missed routine vaccinations.
How Did the Measles Outbreak Get This Bad in Bangladesh?
Bangladesh was once hailed as a vaccination success story. Over two decades of intensive immunisation campaigns reduced measles incidence by more than ninety‑five per cent, positioning Bangladesh as a model for disease control.
Recent cracks in that achievement have emerged. Gaps in vaccination coverage now exist in remote or marginalised communities, where health workers encounter logistical barriers and families remain unreached by routine programmes. Delayed diagnosis, coupled with a fragile emergency response infrastructure, has further eroded the country’s ability to contain the virus swiftly.
High population density in urban centres and densely settled neighbourhoods facilitates rapid person‑to‑person transmission. Malnutrition, prevalent in many low‑income households, worsens clinical outcomes, making infected children more susceptible to severe complications.
Cross‑border movement also contributes to the spread, allowing the virus to traverse national frontiers with ease. Historically, measles outbreaks in Bangladesh have frequently been traced back to clusters of unvaccinated individuals—sometimes entire villages—who slipped through the net of national immunisation efforts.
The central lesson is stark: Measles does not require a nationwide collapse of health services; it only needs a few vulnerable pockets to ignite a wider epidemic.
Global Resurgence Sparks Concern
Bangladesh’s experience is part of a broader, unsettling global trend. Recent estimates suggest that more than ten million people worldwide have contracted measles in a single year, with outbreaks being reported across multiple continents.
Measles stands among the most contagious pathogens known to medicine. In populations lacking vaccination, a single infected individual can transmit the virus to up to eighteen others, underscoring the speed with which outbreaks can accelerate.
Crucially, the majority of recent cases are linked to individuals who are either unvaccinated or insufficiently vaccinated, highlighting a clear pattern: whenever immunisation coverage slips, Measles makes a comeback.
Why This Is a Warning for India
The same risk factors that have fueled Bangladesh’s crisis are present on the other side of the border. India shares densely populated urban agglomerations, migrant communities that are hard to reach, pockets of low immunisation coverage, and high rates of childhood malnutrition. In such an environment, even a modest immunity gap can enable rapid viral spread.
Frequent cross‑border movement, especially in eastern regions, raises the likelihood that the Bangladesh outbreak could spill over into Indian states such as West Bengal, Assam, and the northeastern territories.
Routine immunisation programmes in India experienced significant disruption during the COVID‑19 pandemic, and global vaccination rates have yet to rebound to the ninety‑five per cent coverage needed for herd immunity. As a result, millions of Indian children remain vulnerable.
These conditions create an optimal setting for Measles to re‑emerge, even in a nation with otherwise robust health infrastructure. Perception also plays a dangerous role: Measles is often dismissed as a mild childhood illness. In reality, Measles is one of the most contagious viruses known, and when it strikes undernourished or unvaccinated children, death can follow within a matter of days.
Is the Crisis Preventable?
The unfolding tragedy in Bangladesh is not an inevitability; it is, in fact, preventable. Safe, highly effective Measles vaccines are widely available, yet gaps in coverage—whether due to limited access, inadequate awareness, or complacency—are sufficient to erase decades of progress.
For India, the cautionary signal is unmistakable. The threat of a large‑scale Measles outbreak is not hypothetical; the conditions that have fueled the Bangladesh emergency already exist across Indian borders.
The most direct message for parents is clear: ensure that every child receives the full Measles vaccination schedule. Achieving and maintaining high coverage rates will re‑establish the community immunity needed to keep Measles at bay.
Beyond individual actions, health authorities must reinforce outreach to marginalized communities, strengthen surveillance systems for early case detection, and guarantee rapid response capabilities to contain any flare‑ups before they expand.
Only through coordinated, sustained effort can the momentum of Measles resurgence be halted, safeguarding the health of children throughout Bangladesh, India, and the wider world.